Chronic Kidney Disease: A Silent Threat
Chronic kidney disease (CKD) is a progressive loss of kidney function over time. It’s a significant public health problem affecting millions worldwide, often going undetected until it reaches advanced stages. This article delves into the intricacies of CKD, covering its causes, stages, symptoms, diagnosis, treatment, and management.
Before exploring CKD, it’s crucial to understand the vital role kidneys play in maintaining overall health. These bean-shaped organs, located on either side of the spine below the rib cage, perform several essential functions:

Filtering Waste Products: Kidneys remove metabolic waste products, such as urea and creatinine, from the blood.
When kidney function declines, these vital processes are disrupted, leading to a cascade of health problems.
Several factors can contribute to the development of CKD. Common causes include:
Diabetes
Diabetes is a leading cause of CKD. High blood sugar levels can damage the blood vessels in the kidneys, impairing their filtering ability.
High Blood Pressure (Hypertension)
Elevated blood pressure can strain the kidneys’ blood vessels, leading to progressive damage.
Glomerulonephritis
This group of diseases involves inflammation of the glomeruli, the tiny filtering units in the kidneys.
Polycystic Kidney Disease (PKD)
PKD is a genetic disorder characterized by the growth of cysts in the kidneys, eventually leading to kidney failure.
Obstructions in the Urinary Tract
Conditions like kidney stones, tumors, or an enlarged prostate can block the flow of urine, causing kidney damage.
Reflux Nephropathy
This occurs when urine flows backward from the bladder into the kidneys, leading to infections and scarring.
Certain Medications and Toxins
Prolonged use of some medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), and exposure to toxins can damage the kidneys.
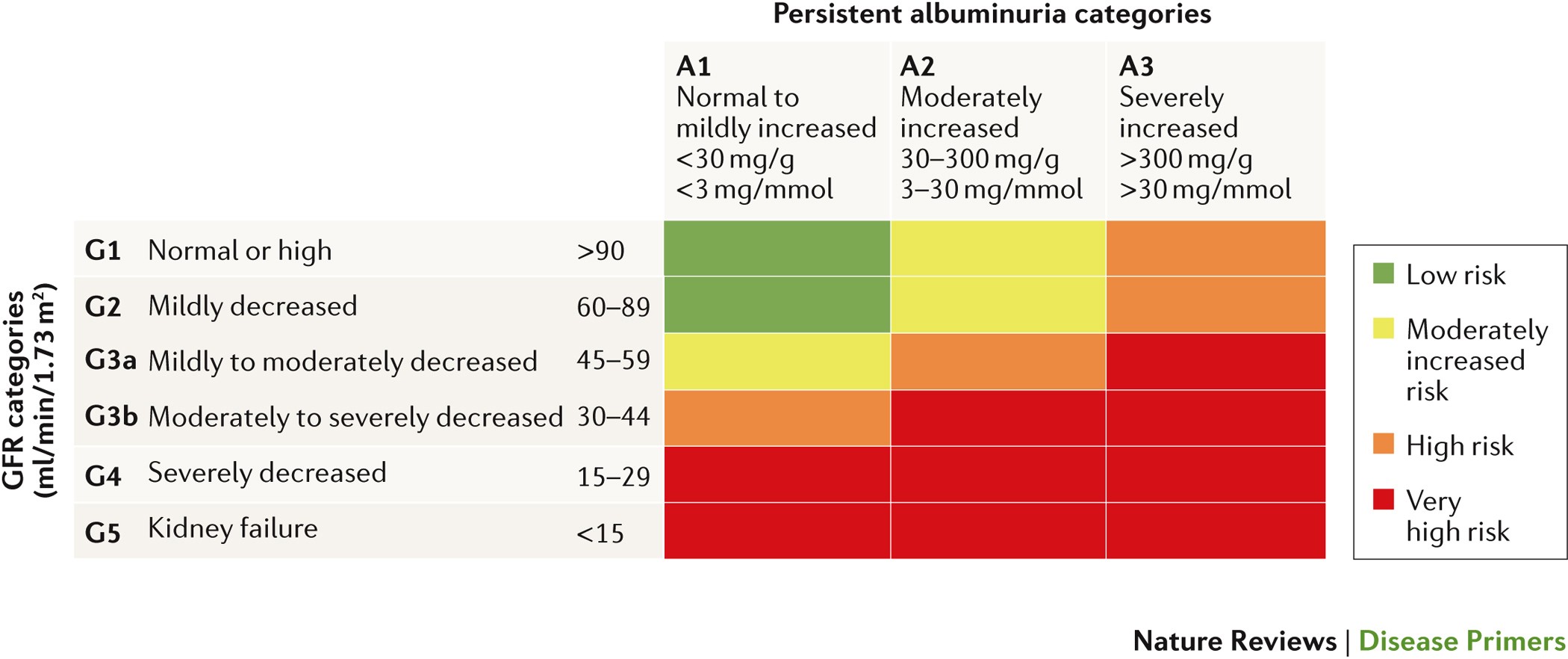
CKD is classified into five stages based on the estimated glomerular filtration rate (eGFR), which measures kidney function:
Stage 1: eGFR ≥ 90 mL/min/1.73 m²
Kidney damage with normal or increased eGFR. At this stage, there may be no noticeable symptoms.
Stage 2: eGFR 60-89 mL/min/1.73 m²
Mild reduction in eGFR. Some subtle changes in kidney function may be present.
Stage 3a: eGFR 45-59 mL/min/1.73 m²
Moderate reduction in eGFR. Symptoms may begin to appear.
Stage 3b: eGFR 30-44 mL/min/1.73 m²
Moderate to severe reduction in eGFR. Symptoms become more pronounced.
Stage 4: eGFR 15-29 mL/min/1.73 m²
Severe reduction in eGFR. Preparation for kidney replacement therapy (dialysis or transplantation) may be necessary.
Stage 5: eGFR < 15 mL/min/1.73 m² (End-Stage Renal Disease or ESRD)
Kidney failure. Kidney replacement therapy is required for survival.
In the early stages, CKD often presents with few or no symptoms. As kidney function declines, the following symptoms may develop:
Fatigue and Weakness: Reduced production of EPO can lead to anemia, causing fatigue and weakness.
Early detection of CKD is crucial for slowing its progression and preventing complications. Diagnostic tests include:
Blood Tests: Measuring creatinine and eGFR to assess kidney function.
Treatment for CKD focuses on slowing the progression of the disease, managing symptoms, and preventing complications.
Managing Underlying Causes
Controlling blood sugar in diabetic patients and managing high blood pressure are essential for slowing CKD progression.
Medications
Dietary Changes
Lifestyle Modifications
Kidney Replacement Therapy
In advanced stages (ESRD), kidney replacement therapy is necessary for survival. Options include:
Hemodialysis
A machine filters waste products and excess fluid from the blood.
Peritoneal Dialysis
A solution is infused into the abdomen to absorb waste products and excess fluid.
Kidney Transplantation
A healthy kidney from a donor is surgically implanted.
CKD can lead to several complications, including:
Anemia: Reduced production of EPO.
Preventing CKD involves managing risk factors and adopting healthy lifestyle habits:
Controlling blood sugar levels: For individuals with diabetes.
Living with CKD requires ongoing management and support. It’s essential to:
Work closely with healthcare providers: To develop a comprehensive treatment plan.
Chronic kidney disease is a serious condition that requires ongoing management. Early detection and intervention can significantly improve outcomes and quality of life. By understanding the causes, stages, symptoms, and treatment options, individuals can take proactive steps to protect their kidney health.



