Decoding the Aches: A Comprehensive Guide to Muscle Pain
Muscle pain, or myalgia, is an incredibly common ailment, affecting people of all ages and activity levels. From a mild twinge after a workout to debilitating chronic pain, the spectrum of muscle discomfort is vast. This comprehensive guide aims to shed light on the various aspects of muscle pain, exploring its causes, symptoms, diagnosis, and management.
Muscle pain arises from irritation or injury to the muscles, tendons, or ligaments. These structures are integral to movement and support, and when compromised, they can cause significant discomfort. Myalgia can be localized, affecting a specific area, or generalized, impacting multiple muscle groups throughout the body.
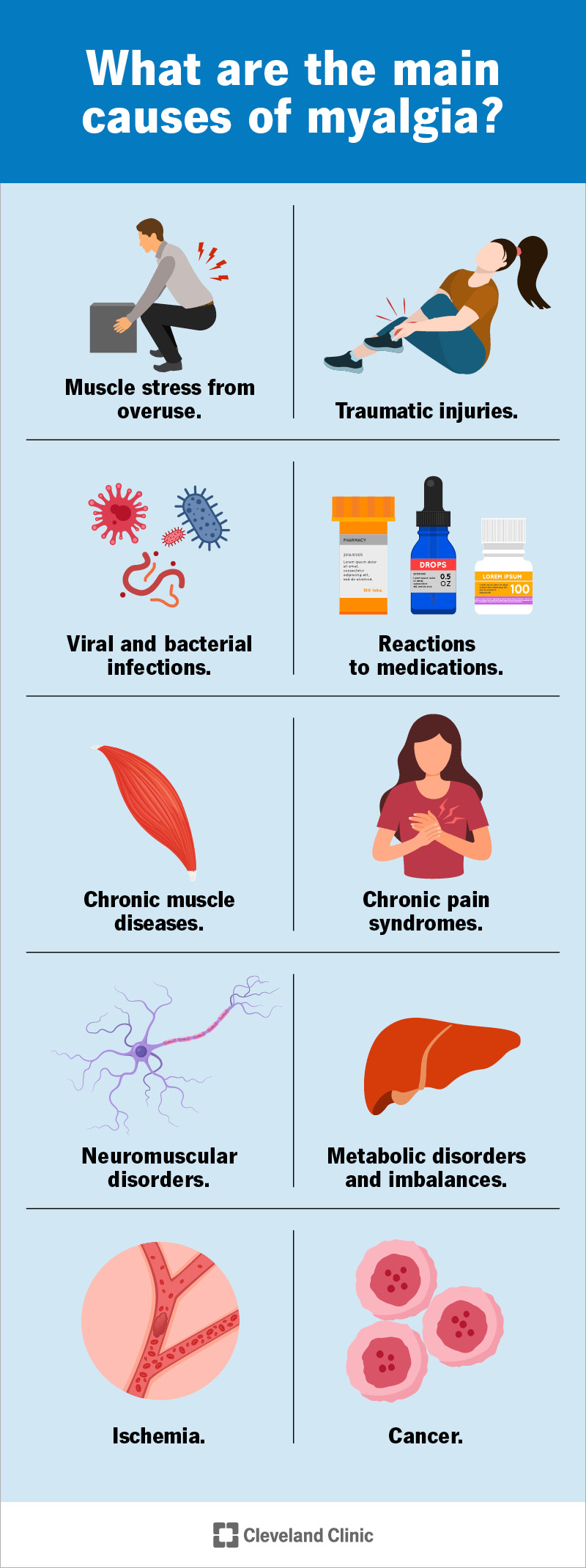
1. Overuse and Strain: The Athlete’s Bane (and Everyone Else’s Too)
One of the most frequent culprits is overuse or strain. This occurs when muscles are pushed beyond their normal capacity, leading to microscopic tears and inflammation. Activities like intense exercise, heavy lifting, or repetitive motions can contribute to this type of pain.
Delayed-Onset Muscle Soreness (DOMS): This is a specific type of muscle pain that develops 24-72 hours after strenuous exercise. It is characterized by stiffness, tenderness, and reduced muscle strength.
2. Injuries: Trauma and Beyond
Direct trauma, such as falls, blows, or accidents, can cause muscle contusions, tears, and even ruptures. These injuries can lead to significant pain, swelling, and limited mobility.
Contusions (Bruises): These occur when blood vessels are damaged, leading to bleeding into the surrounding tissues.
3. Infections: When Your Body Fights Back
Various infections can trigger muscle pain as a systemic response.
Viral Infections: Common viral infections like the flu, common cold, and COVID-19 can cause generalized muscle aches and pains.
4. Autoimmune Diseases: When the Body Attacks Itself
In autoimmune diseases, the immune system mistakenly attacks healthy tissues, including muscles.
Polymyositis and Dermatomyositis: These are inflammatory muscle diseases characterized by muscle weakness and pain.
5. Medications: Side Effects and Interactions
Certain medications can cause muscle pain as a side effect.
Statins: These cholesterol-lowering drugs can sometimes cause muscle aches and weakness.
6. Neurological Conditions: The Nerve Connection
Nerve-related conditions can also manifest as muscle pain.
Fibromyalgia: This chronic condition is characterized by widespread muscle pain, fatigue, and sleep disturbances.
7. Electrolyte Imbalances: The Body’s Chemistry
Imbalances in electrolytes, such as potassium, calcium, and magnesium, can affect muscle function and cause pain.
Hypokalemia (Low Potassium): Can lead to muscle weakness, cramps, and pain.
8. Other Causes: Diverse Triggers
Stress and Tension: Psychological stress can lead to muscle tension, particularly in the neck and shoulders.
The symptoms of muscle pain can vary depending on the underlying cause. Common symptoms include:
Aching or Soreness: A dull, persistent pain in the affected muscles.
Diagnosing muscle pain involves a thorough medical history, physical examination, and sometimes, further investigations.
Medical History: The doctor will ask about the onset, duration, and characteristics of the pain, as well as any other symptoms.
The treatment of muscle pain depends on the underlying cause. Common treatment approaches include:
1. Rest and Ice: The First Line of Defense
For acute muscle pain due to overuse or strain, rest and ice are often effective.
Rest: Avoid activities that aggravate the pain.
2. Heat Therapy: Soothing Relief
Heat therapy can help relax tense muscles and relieve pain.
Warm Baths or Showers: Soaking in warm water can provide relief.
3. Pain Relievers: Over-the-Counter and Prescription
Over-the-Counter Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen can help reduce pain and inflammation. Acetaminophen can also help relieve pain.
4. Physical Therapy: Restoring Function
Physical therapy can help improve muscle strength, flexibility, and range of motion.
Exercises: Targeted exercises can help strengthen and stretch muscles.
5. Medications for Specific Conditions: Addressing the Root Cause
Antibiotics: For bacterial infections.
6. Lifestyle Modifications: Long-Term Management
Regular Exercise: Engage in regular physical activity to maintain muscle strength and flexibility.
While most muscle pain resolves with home care, it’s important to seek medical attention if:
The pain is severe or persistent.
Muscle pain can be a frustrating and debilitating experience. However, by understanding the various causes, symptoms, and treatment options, you can take steps to manage your pain and improve your quality of life. Remember to consult with a healthcare professional for an accurate diagnosis and personalized treatment plan.



